Table of Contents
II. The Different Types of COPD
What is COPD?
Chronic obstructive pulmonary disease, or COPD, is an increasingly common condition in the United States. Over 16 million Americans have been diagnosed with this condition, but many people live with this disease and are unaware. As the name suggests, this disease is chronic and does not have a cure. Once you have COPD, your lungs are permanently damaged, and treatment involves reducing symptoms as much as possible. [1]
Although COPD is common, it is a serious condition that can lead to complications. Having COPD significantly increases your chance of developing lung cancer and heart disease. Luckily, several medications are available to help reduce the side effects of COPD, including Stiolto Respimat, ipratropium/albuterol inhaler, Daliresp (roflumilast), and Atrovent (ipratropium).
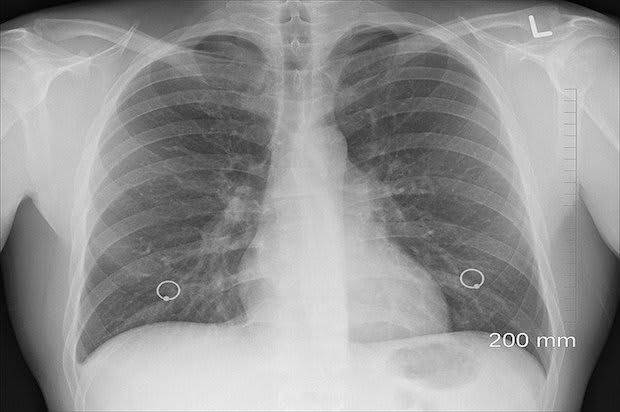
In normally functioning lungs, the air sacs are stretchy and elastic. This elasticity allows the air sacs to expand when you breathe. The air sacs then deflate when you breathe out, expelling carbon dioxide out of your airways. COPD usually occurs due to environmental and lifestyle factors. When your lungs become affected by these factors, several things happen: When all of these things happen, COPD occurs and leads to emphysema or chronic bronchitis. Read on to learn more about COPD and the symptoms and risk factors of this common lung disorder. [2] COPD is a disease that encompasses two conditions: emphysema and bronchitis. Both of these disorders cause airway obstruction, but they affect the lungs in different ways. This lung condition results in shortness of breath due to damaged air sacs (alveoli). When exposed to irritants over long periods, the alveoli weaken and may rupture completely. This leads to enlarged air sacs, reducing the lungs' surface area and limiting the amount of oxygen in the bloodstream. Having emphysema makes it easier for air to become trapped in the lungs. A persistent cough may also occur from chronic inflammation in the tubes that carry air to the lungs. Symptoms may include: Long-term inflammation of the breathing tubes leads to chronic bronchitis. Those with this type of bronchitis have a cough and excess mucus for most days for at least three months of the year for two years in a row. This condition is most common among smokers and leads to frequent lung infections. Other symptoms may include: Emphysema and chronic bronchitis come with their specific symptoms. Your doctor will determine which condition is affecting your lungs. The unfortunate part of COPD is that symptoms usually do not appear until significant lung damage occurs. The symptoms get worse over time, especially if you continue to smoke. If you are noticing lung problems, you may want to contact your doctor. Look out for: As mentioned earlier, smoking is a major risk factor for COPD, but several other things can increase your likelihood of this disease. The most common risk factors include: Tobacco smoke: Smoking is the number one risk factor for COPD. COPD is most common among long-term cigarette smokers. The longer you smoke, the worse your COPD symptoms may become. Introducing any smoke into the lungs may cause COPD, including pipe, cigar, and marijuana smoking. If you are exposed to secondhand smoking in your household, you may develop COPD as well. Asthma: Having asthma can predispose you to COPD. Asthma is another chronic lung disorder, so it increases your risk of other lung disorders like COPD. Asthma causes your airways to narrow and swell. This can make breathing difficult and is often triggered by certain irritants, like animal dander and smoke. If you smoke and also have asthma, you are much more likely to develop COPD. Exposure to dangerous chemicals: If you work in an environment that exposes you to chemical fumes, vapors, or dust, you are at risk of COPD. Being around these materials day in and day out can irritate and inflame your lungs. Living in a polluted city or poorly ventilated home can also increase your risk of COPD, especially if you burn fuels in your home for cooking. [5] It often takes several doctor visits before COPD is properly diagnosed. If you think you are experiencing a lung problem, you may want to keep a log of your symptoms to present to your doctor. Having a detailed list of your symptoms can help your doctor make a proper diagnosis. Your physician will also ask if you smoke and ask if you are exposed to any lung irritants. Your doctor may order the following tests: Pulmonary function tests: This test determines how much air your lungs can inhale and exhale, determining whether your lungs can supply enough oxygen to the blood. You will blow into a large tube (spirometry test) as hard as you can to measure how much air you can blow out of your lungs. Chest x-ray: Chest x-rays can be used to determine if you are experiencing another lung problem. It can also show the effects of emphysema on the lungs. Lab tests: Your doctor may take a blood sample if you have a family history of COPD. Some people have a genetic disorder, alpha-1-antitrypsin deficiency, which can cause COPD at a young age. Lab tests may also help rule out other conditions and explain some of your symptoms. [5] There are several steps to a successful COPD treatment. The first step usually involves altering your lifestyle so you can avoid as many lung-irritating substances as possible. Your doctor will likely recommend that you stop smoking and avoid being around others who smoke. For many people, quitting smoking can significantly improve their symptoms and slow the progression of COPD. If you have more severe COPD, you may be prescribed medications like Stiolto Respimat, ipratropium/albuterol inhaler, Daliresp (roflumilast), and the Atrovent (ipratropium) inhaler. You may be prescribed inhalers that relax the muscles in the airways and make breathing easier. Inhaled steroid medications can also reduce airway inflammation and prevent frequent COPD exacerbation. If your COPD is more severe, you may also be given oxygen therapy and may have to undergo a pulmonary rehabilitation program. Your doctor will determine the best treatment for you. [5] The content in this article is intended for informational purposes only. This website does not provide medical advice. In all circumstances, you should always seek the advice of your physician and/or other qualified health professionals(s) for drug, medical condition, or treatment advice. The content provided on this website is not a substitute for professional medical advice, diagnosis, or treatment.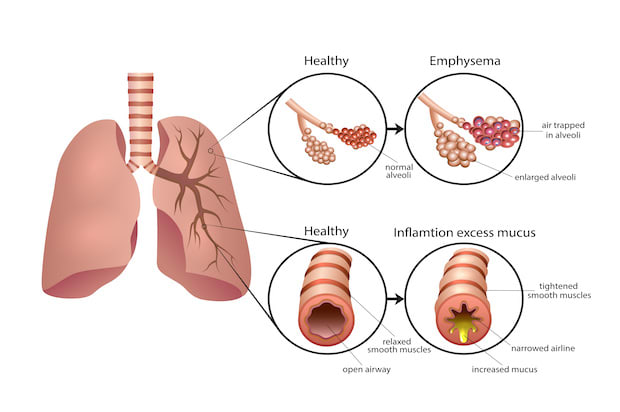
The Different Types of COPD
a. Emphysema
b. Chronic Bronchitis

General Symptoms of COPD
Risk Factors for COPD
Diagnosing COPD
Treatment
